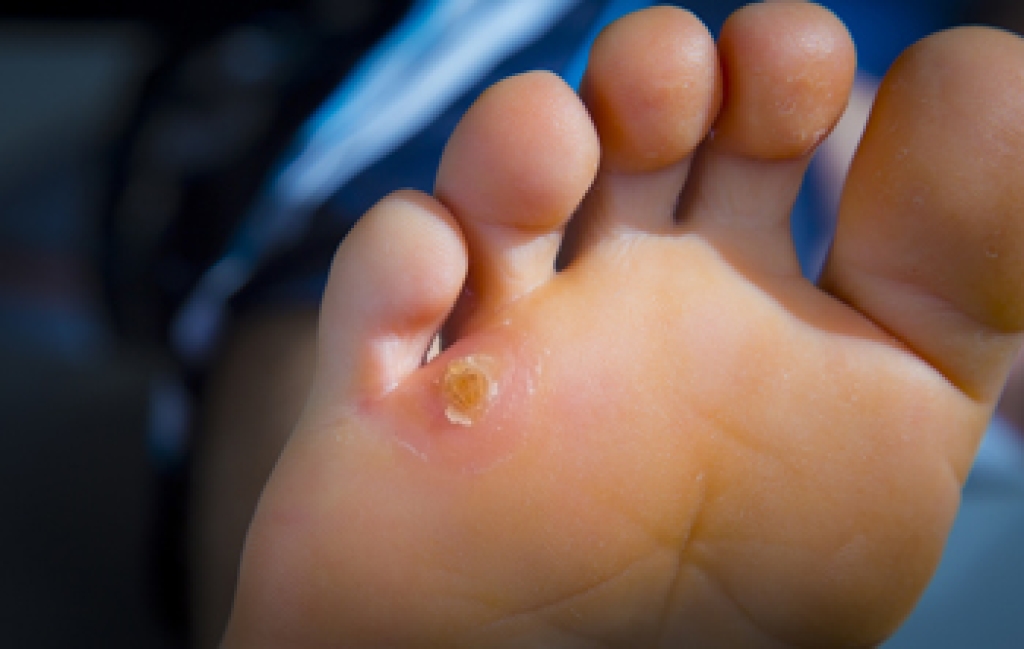
Corns are thickened areas of skin that form due to constant friction or pressure, often from wearing tight shoes or abnormal foot structure. The two main types are hard corns and soft corns. Hard corns typically develop on the top or tip of the toes and contain a dense core of dead skin that can cause pain while walking. Soft corns, also called interdigital corns, usually form between the toes, especially the fourth and fifth toes, where moisture keeps them pliable but still painful. Corns differ from calluses in that calluses are larger, flatter, and tend to form on weight-bearing areas such as the balls of the feet. A podiatrist can assess the cause of corns and provide safe treatment by trimming thickened skin, removing the core, or recommending surgery, if necessary. Recurrent or painful corns may indicate underlying foot deformities that can be addressed by a podiatrist. If you have a painful corn on your foot, it is suggested that you schedule an appointment with a podiatrist for safe and sterile treatment.
If you have any concerns regarding your feet and ankles, contact Jeffrey Parrett, DPM of Parrett Podiatry. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions, please feel free to contact our office located in Waxahachie, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.